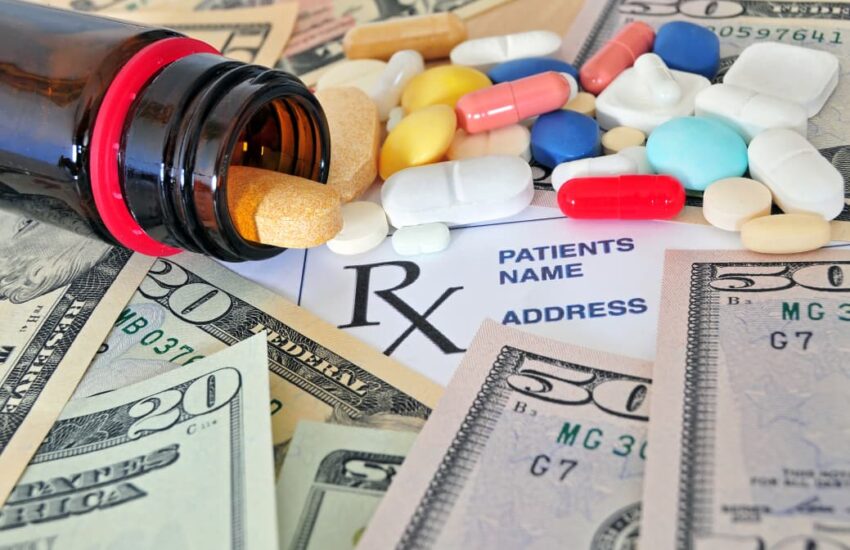
Let me tell you something that most of us get wrong when we are shopping for health insurance. We look at the monthly premium, we glance at the deductible, and we make a decision. That is pretty much it. The prescription drug coverage part? That usually gets about five seconds of our attention before we move on to something more interesting, like what we are having for dinner.
I have been guilty of this myself. A few years back, I was switching plans during open enrollment and found what looked like a steal. The monthly payment was low, the deductible was manageable, and I clicked enroll without a second thought. Six months later, I needed medication that was not on the formulary. That cheap plan suddenly did not feel so cheap anymore.
Here is the thing about health insurance in the United States. Thanks to the Affordable Care Act, most plans have to cover prescription drugs to some degree. But that word “some” is doing a lot of heavy lifting. The reality is that coverage varies wildly from one plan to the next. You have to dig into what is actually covered, which drugs make the cut, and how much you will be paying when you walk up to the pharmacy counter.
Insurance companies organize their drug coverage using something called a formulary. Think of it as a list with different levels, or tiers. Tier one is usually generic drugs, and those come with a reasonable copay that does not make you wince. Tier two covers preferred brand-name drugs, which cost more but are still manageable for most people.
Then you hit tier three, the non-preferred brands, and suddenly your wallet starts feeling lighter. Tier four is where things get scary. That is where you find specialty medications, biologics, cancer treatments, and drugs for rare diseases. Some plans require you to pay twenty or even thirty percent of the drug price at that tier. We are talking thousands of dollars a month, even with insurance.
When you are weighing your options during open enrollment, the key is understanding that prescription drug coverage isn’t just a checkbox; it is the difference between affording your medications and skipping doses to get by. The connection between drug coverage and your premium is pretty straightforward.
Plans that make it easy to get your medications, with broad formularies and reasonable copays, cost more each month. Plans that keep the monthly payment low usually do so by cutting corners on drug coverage. Higher copays, narrower lists of covered drugs, and more hoops to jump through with prior authorization.
That plan with the tempting low premium? You have to wonder what they are doing with prescriptions to keep that number so small. I am not making this up. Research from places like the Kaiser Family Foundation backs this up year after year. Health economists have studied what happens when people face high costs for their medications.
The pattern is always the same. People skip doses, they split pills, they stretch refills too far. For chronic conditions like diabetes, high blood pressure, or depression, that is a disaster waiting to happen. You save twenty bucks on a prescription today, and end up in the emergency room six months from now with a problem that costs thousands to fix.
The math does not work in your favor. My advice comes from experience, both personal and from watching friends make the same mistake I did. If you take any medication regularly, and I mean any at all, you should probably choose the plan with better drug coverage, even if the premium is higher. Run the numbers.
Add up what you pay for your current prescriptions over a year. Compare that to what you would pay under a cheaper plan. Factor in the premium difference. The cheap plan often ends up being the expensive choice when you look at the full picture. Of course, there is an exception. If you are genuinely healthy, take no medications, and have not seen a doctor in years, maybe the math shifts a little.
But here is the thing about being healthy. It does not always last. Accidents happen. Illnesses appear. That status can change in a week, sometimes in a day. When it does, you want to be in a plan that has your back. So next time open enrollment rolls around, do yourself a favor. Look past the premium.
Read the fine print on prescription drug coverage. Check the formulary. See what tier your medications fall into. It takes an extra twenty minutes, but those twenty minutes could save you thousands of dollars and a whole lot of stress down the road. I learned that lesson the hard way, so you do not have to.
References
Kaiser Family Foundation. (2023). Prescription Drug Costs in the United States.
U.S. Department of Health and Human Services. (2023). Prescription Drug Coverage and the ACA.
Neuman, T., & Cubanski, J. (2022). Medicare Part D: A First Look at Prescription Drug Plan Availability. Kaiser Family Foundation.